

“Is Sex Supposed to Hurt” is an ongoing series to get unique perspectives on painful sex. Today we’re talking to Abby about her experience with pain during vaginal sex.
From the very first time Abby had vaginal sex she experienced pain. But because she’d heard that was normal, she didn’t think too much about it. After years of pain every time she had sex, Abby eventually decided to seek medical advice. She spent 6 month waitlist to see a specialized gynecologist, and was eventually diagnosed with vestibulodynia/vulvodynia. The recommended treatment was pelvic floor physiotherapy.
With penetration there was always pain at the start, but what happened afterwards would vary. Sometimes it was awful and sharp and it felt like sandpaper on my insides, other times that feeling went away quickly and it was bearable, or even pleasurable, so I had difficulties believing that I needed to get medical attention. And I really wanted to believe it wasn’t anything else, I thought a diagnosis meant I was doomed.
I went to see a doctor, and they told me my problem was that my hymen was thick or something like that. They didn’t really give me a real answer and told me to keep trying and to drink wine to relax. I didn’t see another doctor for another 4 years because I took that answer as fact and just went with it. They told me my only other option was to have my hymen removed, so I decided I’d rather not undergo a surgical procedure that isn’t totally necessary (I’m too worried about complications) and just deal with the way my body was on my own.
I went online to research other people’s experiences and I found that they were more severe. In my case I could still have some penetration and sometimes it was more painful and sometimes it was less painful, it was really inconsistent and hard to describe. But I mostly saw other people talking about vaginismus, which makes any kind of penetration really painful or impossible. That wasn’t my situation, and because I didn’t see myself falling under that diagnosis or condition I still didn’t feel like I had a real problem. I spent a long time doubting it, I thought it was something I could think through or push through. It was ultimately my partner at the time that convinced me to see a doctor again.
It upset me a lot–like why is this happening to me? Sex was supposed to be fun yet it was actually something I began to dread more and more as my discomfort and pain became more severe. More frequently I would have to tell my partner to stop because the pain was too much, and sometimes I would start to cry, not because of the pain itself but from feelings of frustration and guilt. It became especially bad when I learned that I actually have a medical condition. But the more stressed I was about having sex, the more painful it would be. So I ended up deciding to stop having penetrative sex with my partner and to do other things until I could get treatment.
It’s definitely easier to talk about now, it was a thing that made me feel embarrassed and ashamed for a long time especially when I couldn’t put a word on it. I find that being able to have a diagnosis and know that others are going through a similar thing makes me feel better. I would feel really isolated when other people would talk about sex casually. At school my friends would compare their sex lives and talk about the good things and it would make me feel broken. But I actually made an effort to tell people who were more close to me and told my school’s sexual education program to address painful sex as well. If I had known what I was going through earlier I feel like I could’ve dealt with this six years ago. I think awareness is important and I realized how frustrated I was that there was none. And that pelvic pain is a issue that many people come across and that no one talks about. I think it’s more common for people with vaginas, and that we’re also more normalized to the idea of experiencing discomfort and sitting through it. I feel passionate about it in a way now but only because I was so ashamed about it before.
So I’m being treated for vestibulodynia/vulvodynia that just means means having pain in specific areas of the vulva and vagina, for me it’s the entrance area mostly. A lot of general disorders in the vaginal area involve pelvic floor muscles, mine are too tense and it’s really exacerbated by stress and anxiety. My partner would point out that was trend too. It’s definitely a full psychological and physical thing, and so even without mental stressors, my muscles have already learned to react in a certain way to touch. At first I was prescribed a numbing cream which my partner had to apply and was painful to put on because they had to touch the parts that hurt, it was overall so counterintuitive and didn’t work that well. For other people that treatment works, depending on the nature of their condition but for me it did not. I’m currently doing pelvic floor physiotherapy.
I was asked like a million questions and had to fill out a 10 page questionnaire that they emailed to me before the appointment. The email was actually titled “10 Page Questionnaire” which I found funny. When I actually started the session, the physiotherapist started with checking my back and spine and other muscles in my thighs and butt, observing how sensitive I was to gentle touches. They checked the outside of my vagina with a Q-tip then manually used their hands to check inside my vagina. They were able to tell me specifically that my tension was on the left side–“if you see it as a circle we can locate your muscle tension at 4 o’clock”. They spent time doing massages just like you would for any other kind of muscle tension basically. We just chatted while that was happening, like while their hands were casually inside me. There’s actually like a sheet that they put over my lower half but it was kind of unnecessary because if I had to turn on my side or anything I was totally exposed except for this sheet wedged between my legs. Anyways, I was given some exercises to do at home like 10 times a day. It is phsyio in a “normal” sense, I found the whole thing pretty comfortable. Part of why it was okay is because I already had a lot of examinations by general practitioners and gynecologists, and I was told in advance that on a scale of 1-10 pain/discomfort shouldn’t go past a 3.
The physiotherapy is pretty expensive. I’m not covered, I don’t have real insurance I have like student insurance which covers 80% for up to $300 in a year. Luckily, the doctor said for my case I wouldn’t need too many sessions like 6-8. My initial assessment was $180 and that was an hour, and continuing with half hour physio sessions will be $85/session. It costs a lot so I hope it works.
I think I have a lot of learning to do when it comes to experiencing sexual pleasure with a partner. And I definitely don’t feel included in the conversations surrounding sex positivity. I want to have sex but it’s so complicated. I feel left out by how much people emphasize sex. Everything surrounding sex is not just physically but emotionally difficult for me. Being tied up in these experiences I’ve had with pain over the years I know that casual sex isn’t really an option for me right now and I don’t know if it’s something I want in the future. It’s like I’m starting from ground zero. Perhaps my expectations of how much it will improve are too high, but I’m glad I’m finally doing something about my sexual health and pleasure even though it’s taken a long long time.
Please note that some of these articles use gendered language when talking about bodies.
If you have questions about this topic, feel free to contact one of our peer educators. [Link]
Last Updated: April 2020
Going on hormones is supposed to change your body and that can be pretty scary when you don’t know what to expect. For this post, we’ve adapted a some resources from the Rainbow Health Network’s pages on Feminizing and Masculinizing Hormone Therapy.

Winnie Wang is latest subject in our 5 Questions With series, and they’re here to talk with us about what it’s like to be a non-binary person in gendered spaces.
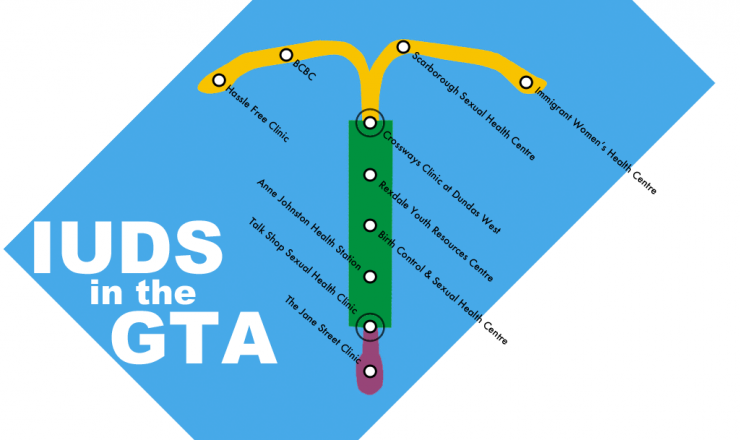
Check out this list of health clinics in the GTA who sell and do IUD insertions across the city.